Understanding the Stages 4 Endometriosis
Stage 4 endometriosis represents the most extensive form of the disease, marked by widespread lesions, deep infiltration, and significant adhesions involving multiple pelvic organs. At this stage, endometrial-like tissue may heavily distort normal anatomy and contribute to severe symptoms or fertility challenges. The following section explains what defines Stage 4 disease and how it impacts the body.
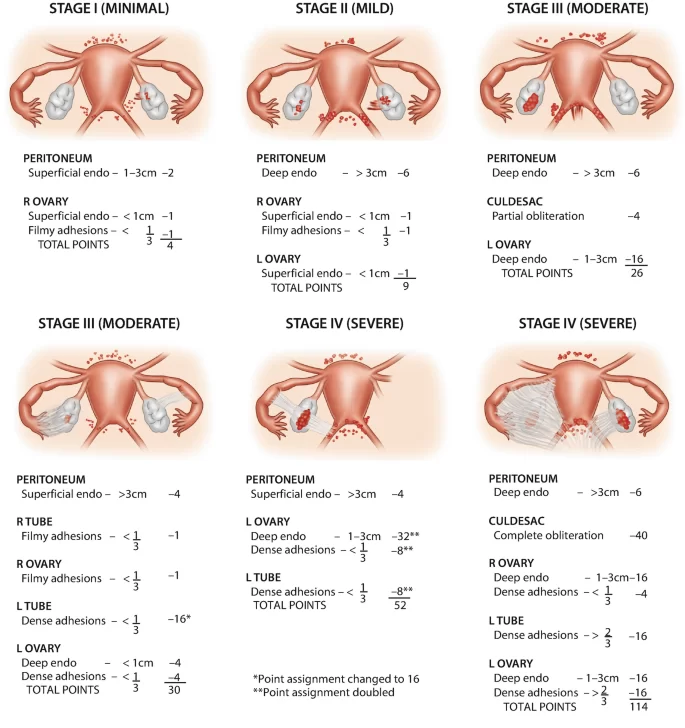
This chart represents the rASRM scoring criteria for Stage IV endometriosis, the severe stage of the condition.
Stage IV is characterized by extensive deep implants, large endometriomas, and dense adhesions that may fuse pelvic organs together. The scoring reflects the highest level of structural involvement and disease spread.
Even at this advanced stage, symptoms do not always correspond to the severity of findings — some individuals have intense pain, while others may have minimal discomfort.
COMMON QUESTIONS ABOUT Stage 4 Endometriosis
Stage 4 endometriosis is the most severe stage of endometriosis, a condition in which the tissue similar to the lining of the uterus, called the endometrium, grows outside the uterus. In stage 4 endometriosis, the implants of endometrial tissue are deeply infiltrating and widespread. These implants may be found not only in the pelvic region but also on other organs such as the ovaries, fallopian tubes, bladder, intestines, and even the diaphragm.
The severity of stage 4 endometriosis is determined by the extent of the implants and the presence of adhesions, which are abnormal bands of scar tissue that can cause organs to stick together. The implants and adhesions can lead to severe pain, inflammation, and distortion of the affected organs. Stage 4 endometriosis may also be associated with complications like ovarian cysts (endometriomas) and infertility.
Stage 4 endometriosis, being the most severe stage of the condition, is often associated with a range of pronounced and debilitating symptoms. These symptoms can vary from person to person, but common manifestations of stage 4 endometriosis may include:
- Chronic Pelvic Pain: Women with stage 4 endometriosis often experience intense and persistent pelvic pain that may worsen during menstruation or intercourse. The pain may also be present throughout the menstrual cycle.
- Dysmenorrhea: Stage 4 endometriosis is frequently accompanied by severe menstrual cramps, known as dysmenorrhea. These cramps can be debilitating and may interfere with daily activities.
- Painful Intercourse (Dyspareunia): The presence of endometrial implants and adhesions in the pelvic region can lead to pain or discomfort during sexual intercourse.
- Gastrointestinal Disturbances: Endometrial implants on the intestines or other abdominal organs can cause gastrointestinal symptoms such as bloating, constipation, diarrhea, nausea, and rectal pain.
- Urinary Issues: Endometriosis affecting the bladder or ureters can result in urinary symptoms such as frequent urination, urgency, pain or discomfort during urination, or blood in the urine.
- Fatigue: Chronic pain and the impact on overall health can contribute to fatigue and a general feeling of low energy.
- Fertility Problems: Stage 4 endometriosis is associated with a higher likelihood of infertility or difficulty in conceiving due to the distortion and blockage of the reproductive organs.
It is important to note that the severity of symptoms can vary among individuals, and some women with stage 4 endometriosis may experience more or fewer symptoms than others. Additionally, the presence and intensity of symptoms may not necessarily correlate with the stage of endometriosis, as symptom severity can be influenced by various factors, including individual pain tolerance and the location of endometrial implants. Proper diagnosis and consultation with a healthcare professional are crucial for evaluating symptoms and determining the appropriate management plan for stage 4 endometriosis.
Life-threatening Complications in Stage 4 Endometriosis
Stage 4 endometriosis, as a standalone condition, is not directly linked to death. However, in rare cases, severe complications arising from stage 4 endometriosis can potentially lead to life-threatening situations. These complications are extremely uncommon, but they include scenarios such as ovarian endometrioma rupture, bowel obstruction or perforation, or kidney involvement.
In such cases, immediate medical attention and intervention are necessary to prevent life-threatening consequences. It is important to note that with proper medical management, including timely diagnosis, effective pain management, and surgical intervention when needed, the majority of women with stage 4 endometriosis can lead productive lives and successfully manage their condition.
It is crucial for individuals experiencing symptoms or concerns related to endometriosis to request an appointment with New York Gynecology Endometriosis (NYGE) for proper evaluation, diagnosis, and management to ensure the best possible outcomes.
Diagnosing stage 4 endometriosis typically involves a combination of medical history assessment, physical examinations, imaging techniques, and, in many cases, surgical exploration. Here is an overview of the diagnostic approaches commonly used:
- Medical History Assessment: The healthcare provider will start by discussing the patient’s symptoms, including the nature, duration, and intensity of pelvic pain, menstrual abnormalities, and other related symptoms. A detailed medical history helps in evaluating the likelihood of endometriosis and ruling out other possible conditions.
- Physical Examination: A pelvic examination is performed to assess the pelvic organs for any abnormalities, such as the presence of masses, tenderness, or nodules. However, it’s important to note that physical examination alone cannot definitively diagnose endometriosis.
- Imaging Techniques: Various imaging modalities may be used to support the diagnosis of endometriosis. These include:
- Transvaginal Ultrasound: This type of ultrasound is conducted by inserting a small probe into the vagina to visualize the pelvic organs. It can help detect ovarian cysts (endometriomas) and identify large endometrial growths or adhesions
- Magnetic Resonance Imaging (MRI): An MRI scan may be recommended to obtain detailed images of the pelvic region. It can help visualize endometrial implants, adhesions, and their involvement with surrounding organs.
- Laparoscopy: Laparoscopy is considered the gold standard for diagnosing endometriosis, including stage 4. It is a surgical procedure performed under general anesthesia. The surgeon makes small incisions in the abdomen and inserts a thin, lighted instrument called a laparoscope to visualize the pelvic organs directly. During laparoscopy, the surgeon can identify and classify the extent of endometrial implants, adhesions, and other abnormalities associated with endometriosis. Biopsy samples may also be taken for confirmation of the diagnosis.
It’s important to note that the definitive diagnosis of endometriosis, including stage 4, can only be made through laparoscopy and histological examination of the tissue samples obtained during the procedure.
Patients in Babylon and Bay Shore, NY facing Stage 4 endometriosis turn to NYGSE for highly specialized care, where complex cases are evaluated in depth and treated with advanced surgical expertise close to home.
Surgical Treatment for Stage 4 Endometriosis
Surgical treatment plays a significant role in managing stage 4 endometriosis. As the most severe form of the condition, stage 4 endometriosis often requires surgical intervention to alleviate symptoms, address complications, and improve the quality of life for affected individuals. The surgical approaches used for stage 4 endometriosis can vary depending on the specific circumstances and goals of the patient.
Here are some common surgical treatments for stage 4 endometriosis:
Laparoscopic surgery, also known as minimally invasive surgery, is a common approach for treating stage 4 endometriosis. During the procedure, small incisions are made in the abdomen, and a laparoscope (a thin, lighted instrument) is inserted to visualize the pelvic organs. The surgeon then excises or removes the endometrial implants, adhesions, and scar tissue. Laparoscopic excision aims to alleviate pain, restore organ function, and improve fertility when applicable.
According to Healthcare Bluebook, the cost of laparoscopic excision of endometriosis can vary depending on the location, healthcare provider, and type of insurance. On average, the cost of the procedure can range from $4,000 to $15,000. It’s important to note that these are estimated costs and may not reflect the actual cost you may incur.
To obtain an accurate cost estimate, it is advisable to request an appointment with New York Gynecology Surgery & Endometriosis (NYGSE).
In cases where stage 4 endometriosis is causing severe symptoms, impacting multiple organs, or if fertility preservation is not a concern, a hysterectomy may be recommended. A hysterectomy involves the removal of the uterus and, in some cases, may also include the removal of the ovaries and fallopian tubes (salpingo-oophorectomy). This surgical option can be an effective solution for managing endometriosis-related pain and reducing the risk of recurrence.
According to a report by the Healthcare Cost and Utilization Project (HCUP), the average cost of a hysterectomy in the United States ranges from $5,000 to $12,000. However, this is an average estimate and does not include additional expenses such as pre-operative consultations, lab tests, anesthesia fees, hospital stay, medications, and post-operative care.
Bowel resection is a surgical procedure that may be required in cases of stage 4 endometriosis when the endometrial implants infiltrate the intestines or cause significant complications such as bowel obstruction or perforation. This specialized surgical intervention aims to remove the affected portion of the bowel and restore normal bowel function.
In stage 4 endometriosis, endometrial implants can invade the walls of the intestines, leading to adhesions, scar tissue, and potential bowel complications. Symptoms such as severe abdominal pain, bowel obstruction, rectal bleeding, or perforation may indicate the need for bowel resection.
Bowel resection in stage 4 endometriosis requires specialized surgical skills and may involve a multidisciplinary approach with gynecologists and colorectal surgeons working together to address the complex nature of the condition.
Pankaj Singhal, MD, MS, MHCM
With over 12 years of experience in both academic and private healthcare, Dr. Singhal has trained more than 45 gynecologic surgeons and fellows in minimally invasive and oncologic procedures. He has pioneered new surgical techniques for endometriosis and laparoscopic surgery, completing more than 5,700 robotic-assisted cases nationwide. Renowned for taking on the most complex cases other centers turn away, Dr. Singhal continues to advance the standard of women’s surgical care.
