Deep Infiltrating Endometriosis (DIE)
Deep infiltrating endometriosis (DIE) is one of the most severe forms of endometriosis, defined by lesions that penetrate several millimeters or more into surrounding organs and tissues. Unlike superficial disease, DIE often involves critical structures such as the bowel, bladder, ureters, uterosacral ligaments, and pelvic nerves. Because these lesions trigger chronic inflammation, scarring, adhesions, and sometimes organ dysfunction, DIE is frequently associated with severe pain, gastrointestinal or urinary symptoms, and infertility. Accurate diagnosis and treatment require evaluation by specialists experienced in advanced endometriosis care.
Illustration showing endometrial implants affecting the ovaries, fallopian tubes, and pelvic structures. Deep infiltrating endometriosis extends beyond superficial surfaces and can invade vital tissues, contributing to pain, inflammation, and organ dysfunction.
COMMON QUESTIONS ABOUT DEEP Infiltrating Endometriosis
Deep infiltrating endometriosis (DIE) is considered a highly invasive form of endometriosis due to its ability to penetrate deeply into the surrounding tissues and organs. It is characterized by the growth of endometrial tissue outside the uterus, typically in the pelvic region, but can also affect other areas of the body.
Endometriosis itself is a condition in which the tissue that normally lines the uterus (endometrium) grows outside of it. In the case of deep infiltrating endometriosis, this misplaced endometrial tissue infiltrates and implants into the surrounding structures, such as the pelvic cavity, ovaries, fallopian tubes, bladder, and bowel.
Several factors contribute to the invasiveness of deep infiltrating endometriosis:
Depth of infiltration: Unlike superficial endometriosis, which affects the outermost layers of tissue, deep infiltrating endometriosis infiltrates deeply into the tissues and organs. It can penetrate several millimeters or even centimeters beneath the surface, leading to significant involvement and adhesion formation.
Invasion of surrounding structures: Deep infiltrating endometriosis can invade nearby organs and tissues, such as the bowel or bladder. The abnormal growth of endometrial tissue can cause adhesions, scarring, and structural changes in these organs, leading to pain, inflammation, and other symptoms.
Inflammatory response: The presence of endometrial tissue outside the uterus triggers an inflammatory response in the affected areas. Chronic inflammation can lead to tissue damage, fibrosis, and further invasion of surrounding tissues.
Nerve involvement: Deep infiltrating endometriosis can affect nerves in the pelvic region, leading to severe pain and discomfort. The infiltrating tissue can irritate or compress the nerves, causing persistent pain even in the absence of menstrual bleeding.
The exact causes of Deep Infiltrating Endometriosis (DIE) are not fully understood, but there are several theories that help explain its development.
One prominent theory is retrograde menstruation, which suggests that during menstruation, menstrual blood containing endometrial cells flows backward through the fallopian tubes into the pelvic cavity instead of exiting the body. These displaced endometrial cells can then implant and grow on the pelvic organs, leading to the development of endometriosis, including the deep infiltrating form. However, retrograde menstruation alone cannot fully explain the occurrence of DIE, as many women experience retrograde menstruation without developing the condition.
Other contributing factors may include hormonal imbalances, genetic predisposition, impaired immune system function, and environmental factors. Hormones such as estrogen are known to stimulate the growth of endometrial tissue. Therefore, hormonal imbalances or abnormalities could promote the development and progression of endometriosis. Genetic factors may also play a role, as endometriosis tends to run in families, suggesting a hereditary component. Additionally, certain environmental factors, such as exposure to toxins or chemicals, could potentially influence the development of endometriosis, although more research is needed to establish a definitive link.
It’s important to note that while these theories provide some insight into the potential causes of deep infiltrating endometriosis, the condition likely results from a combination of multiple factors rather than a single cause. Further research is still needed to fully understand the complex origins of DIE.
Deep Infiltrating Endometriosis (DIE) is associated with a range of symptoms that can significantly impact a person’s quality of life. These symptoms often vary in severity and can include:
- Chronic pelvic pain: Persistent and debilitating pain in the pelvic region is a common symptom of DIE. The pain may worsen during menstruation, sexual intercourse (dyspareunia), or bowel movements. It can also be present throughout the menstrual cycle and may extend to the lower back and thighs.
- Gastrointestinal disturbances: Deep infiltrating endometriosis can affect the gastrointestinal tract, leading to symptoms such as bloating, diarrhea, constipation, nausea, and abdominal cramps. Some individuals may also experience rectal bleeding or pain during bowel movements.
- Urinary symptoms: DIE can involve the urinary system, resulting in symptoms like frequent urination, urgency, pain during urination, or blood in the urine.
- Infertility: Deep infiltrating endometriosis is associated with fertility problems. The abnormal growth and scarring caused by endometriosis can obstruct the fallopian tubes or affect the quality of the eggs or sperm, making it more difficult to conceive.
- Painful intercourse: Deep infiltrating endometriosis can cause deep pelvic pain during sexual intercourse, which is known as dyspareunia.
It is important to remember that the severity and presentation of symptoms can vary widely among individuals, and some may experience no symptoms at all. Scheduling an appointment with New York Gynecology Surgery & Endometriosis (NYGSE) is crucial for an accurate diagnosis and appropriate management of deep infiltrating endometriosis.
Is Deep Infiltrating Endometriosis life threatening?
Deep Infiltrating Endometriosis (DIE) itself is not typically considered life-threatening. However, it can significantly impact a person’s quality of life and cause chronic pain and other symptoms that can be debilitating. The severity of symptoms can vary among individuals, and some may experience more severe complications related to DIE.
While DIE itself is not life-threatening, complications arising from the condition can have serious implications. For example, if endometriosis infiltrates the bowel, it can lead to bowel obstruction or perforation, requiring medical intervention. In rare cases, extensive DIE involvement in vital organs or structures can cause severe complications, but such instances are uncommon.
It’s important for individuals with deep infiltrating endometriosis to receive appropriate medical care and management to alleviate symptoms, minimize complications, and improve their overall well-being. Regular follow-ups with healthcare providers and adherence to treatment plans can help address the impact of DIE on daily life and reproductive health.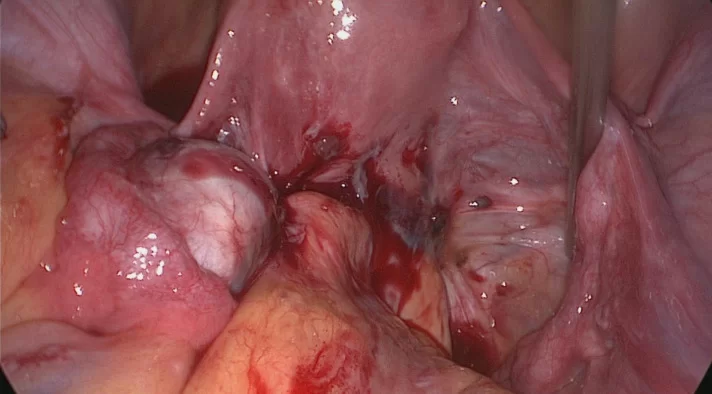
The diagnosis of deep infiltrating endometriosis (DIE) typically involves a combination of medical history evaluation, physical examination, imaging studies, and surgical procedures. Here is an overview of the diagnostic methods commonly used:
- Medical history and symptom assessment: The healthcare provider will gather information about your symptoms, menstrual cycle, pain patterns, and any other relevant medical history.
- Pelvic examination: A pelvic examination may be performed to check for any abnormalities, tenderness, or masses in the pelvic region.
- Imaging studies: Imaging techniques such as transvaginal ultrasound (TVUS) or pelvic MRI (magnetic resonance imaging) can help visualize the pelvic structures and detect the presence of endometrial growths or adhesions. These imaging modalities can provide valuable information about the location and extent of the endometriosis.
- Laparoscopy: Laparoscopy is a surgical procedure considered the gold standard for diagnosing endometriosis, including deep infiltrating endometriosis. It involves making small incisions in the abdomen to insert a laparoscope (a thin, lighted tube with a camera) to visualize the pelvic organs directly. During laparoscopy, the surgeon can identify and evaluate the location, size, and depth of the endometrial lesions, and may also perform biopsies for confirmation.
It’s important to note that definitive diagnosis of deep infiltrating endometriosis can only be made through surgical intervention, typically laparoscopy. Other diagnostic methods, such as imaging, can provide supportive evidence but may not offer a conclusive diagnosis.
Diagnosing deep infiltrating endometriosis requires the expertise of a gynecologist or a specialist in reproductive medicine who is experienced in evaluating and treating endometriosis.
Surgical Methods for the Treatment of Deep Infiltrating Endometriosis
The surgical treatment of deep infiltrating endometriosis (DIE) aims to remove or excise the endometrial implants, relieve symptoms, and improve the patient’s quality of life. Several surgical methods may be employed, depending on the location, extent, and severity of the endometriosis lesions.
Here are some common surgical methods used in the treatment of DIE:
Laparoscopic surgery is the preferred approach for treating DIE. It involves making small incisions in the abdomen and inserting specialized surgical instruments, including a laparoscope, to visualize and access the pelvic organs. Using these instruments, the surgeon can carefully excise or remove the endometrial implants and associated scar tissue while preserving healthy tissue.
According to the Healthcare Bluebook, the cost of laparoscopic excision surgery ranges from $6,440 to $20,380, with an average cost of $13,790 in the United States. However, it’s important to note that the actual cost may vary depending on several factors such as the location of the facility, the experience of the surgeon, and the complexity of the procedure. It’s also worth checking with your insurance provider to see what portion of the cost will be covered.
To obtain an accurate cost estimate, it is advisable to make an appointment with NYGSE.
In cases where deep infiltrating endometriosis involves nerves, such as the pelvic nerves or sciatic nerves, nerve-sparing surgical techniques may be employed. The goal is to excise the endometrial lesions while minimizing damage to the nerves and preserving their function.
If deep infiltrating endometriosis affects the bowel, segments of the affected bowel may need to be resected (surgically removed) and reconstructed. This procedure is typically performed by a specialist, such as a colorectal surgeon, in collaboration with a gynecologist.
If the endometrial implants infiltrate the bladder or the ureters (the tubes connecting the kidneys to the bladder), surgical intervention may be required to excise the lesions and restore normal urinary function. This procedure may involve collaboration between urologists and gynecologists.
In cases where other treatments have been unsuccessful, and the patient no longer desires fertility, a hysterectomy (removal of the uterus) may be considered. This procedure can be performed either laparoscopically or through an abdominal incision (laparotomy). In some cases, the removal of the ovaries (oophorectomy) may be recommended as well.
Pankaj Singhal, MD, MS, MHCM
With over 12 years of experience in both academic and private healthcare, Dr. Singhal has trained more than 45 gynecologic surgeons and fellows in minimally invasive and oncologic procedures. He has pioneered new surgical techniques for endometriosis and laparoscopic surgery, completing more than 5,700 robotic-assisted cases nationwide. Renowned for taking on the most complex cases other centers turn away, Dr. Singhal continues to advance the standard of women’s surgical care.
