Understanding the Stages 2 Endometriosis
Stage 2 endometriosis, also known as mild endometriosis, involves small but measurable implants of endometrial tissue on the pelvic lining and organs. Although the disease is still considered early-stage, the lesions are more numerous and slightly deeper than in Stage 1, and mild adhesions may be present. While symptoms can vary widely, many individuals with Stage 2 experience pelvic pain, menstrual discomfort, or early fertility challenges. The following sections explain the characteristics, symptoms, risks, and diagnostic criteria for Stage 2 endometriosis.
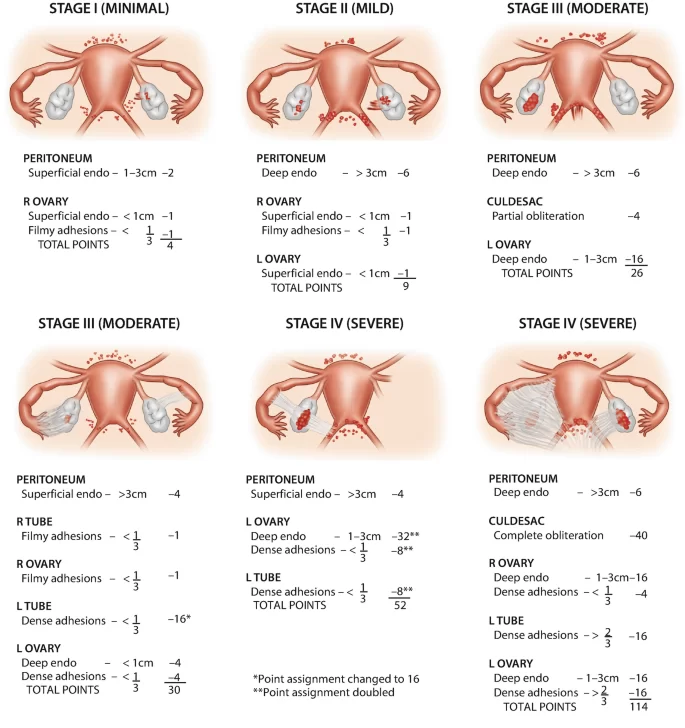
This chart shows how the rASRM scoring system defines Stage II endometriosis, considered mild disease.
Stage II reflects a greater number of implants than Stage I, with some being deeper, and mild adhesions may begin to appear. The system scores lesion size, depth, and the presence of early scar tissue to determine this classification.
Even though Stage II represents a mild level of spread, patient symptoms may be inconsistent and do not always match the staging severity.
COMMON QUESTIONS ABOUT Stage 2 Endometriosis
Stage 2 endometriosis is a classification within the four-stage system used to assess the severity of endometriosis, a chronic medical condition affecting individuals with female reproductive organs. In this stage, the condition is considered to be at a relatively moderate level of progression. It is characterized by the presence of minimal to mild implants of endometrial tissue outside the uterus and pelvic lining.
These implants, also known as lesions or growths, may be found on various pelvic organs and tissues, such as the ovaries, fallopian tubes, and the peritoneum (the lining of the abdominal cavity). Despite their presence outside the uterus, these endometrial tissue growths continue to respond to hormonal changes in the menstrual cycle, causing them to shed and bleed.
However, unlike more advanced stages of endometriosis, stage 2 is associated with fewer and smaller implants, and there may be less overall tissue involvement in the pelvic region. As with all stages of endometriosis, symptoms can vary widely, but they may include pelvic pain, painful menstrual periods, pain during intercourse, and infertility. Early diagnosis and appropriate management are crucial in order to alleviate symptoms and improve the quality of life for individuals with stage 2 endometriosis.
Stage 2 endometriosis, characterized by minimal to mild implants of endometrial tissue outside the uterus and pelvic lining, can present with a range of symptoms that may vary from person to person. Common symptoms of stage 2 endometriosis may include:
- Pelvic Pain: Women with stage 2 endometriosis often experience pelvic discomfort or pain, which can be intermittent or chronic. The pain might be dull, sharp, or cramp-like and can worsen during menstruation, intercourse, or bowel movements.
- Painful Menstruation: Menstrual periods may be accompanied by more intense and prolonged cramps, often starting a few days before the period and lasting throughout its duration.
- Painful Intercourse: Pain or discomfort during sexual intercourse, known as dyspareunia, is a common symptom. It may be felt deep within the pelvis or lower abdomen.
- Gastrointestinal Symptoms: Some individuals might experience gastrointestinal issues such as bloating, constipation, diarrhea, or nausea, particularly around the time of their menstrual cycle.
- Fatigue: Chronic pain and other symptoms can contribute to feelings of fatigue and general tiredness.
- Infertility: Stage 2 endometriosis can affect fertility, as the abnormal tissue growths might interfere with the function of the ovaries, fallopian tubes, or uterus.
- Irregular Bleeding: Women with stage 2 endometriosis might experience irregular menstrual bleeding, spotting between periods, or heavy bleeding.
It’s worth highlighting that the intensity of symptoms is not always directly linked to the stage of endometriosis; individuals with stage 2 endometriosis can encounter varying degrees of symptom severity, ranging from significant discomfort to minimal effects.
If you suspect you may have endometriosis or are experiencing any symptoms of concern, it’s essential to request an appointment with New York Gynecology Surgery & Endometriosis (NYGSE) to seek medical advice and evaluation.
Life-threatening Complications in Stage 2 Endometriosis
While stage 2 endometriosis is generally considered to have a lower risk of life-threatening complications compared to more advanced stages, there are still potential concerns that individuals should be aware of. One notable risk is the potential impact on fertility. Even at this stage, endometriosis can lead to scarring and adhesions that may affect the reproductive organs, potentially leading to difficulties in conceiving and carrying a pregnancy to term.
Another concern is the possibility of severe and chronic pelvic pain. While not life-threatening in itself, this pain can significantly diminish an individual’s quality of life, potentially leading to mental health challenges and a decreased ability to engage in daily activities. Additionally, there is a small chance that endometrial tissue could attach to vital structures such as the intestines or bladder, potentially causing complications such as bowel obstruction or urinary issues. While these risks are relatively uncommon at stage 2, it’s important for individuals with endometriosis to stay informed, seek medical guidance, and explore appropriate treatment options to manage their condition and minimize potential complications.
Diagnosing stage 2 endometriosis involves:
- Clinical Assessment: Your healthcare provider will gather your medical history and discuss your symptoms, focusing on menstrual patterns, pelvic pain, and other relevant information.
- Physical Examination: A pelvic exam may be conducted to check for tender areas, masses, or other signs of endometriosis.
- Imaging: Ultrasound or MRI scans may be used to visualize pelvic structures, helping identify possible endometriosis-related abnormalities.
- Laparoscopy: Considered the definitive diagnostic method, a minimally invasive surgical procedure (laparoscopy) allows direct visualization of pelvic organs, enabling the doctor to identify and evaluate endometriosis lesions. Biopsies can be taken for confirmation.
Early diagnosis and intervention can lead to more effective management and improved quality of life for individuals with endometriosis.
Surgical Treatment for Stage 2 Endometriosis
A common surgical treatment for stage 2 endometriosis is laparoscopic excision or removal of endometrial tissue growths. This minimally invasive procedure aims to alleviate symptoms, improve quality of life, and potentially enhance fertility.
Here’s how surgical treatment for Stage 2 endometriosis is usually conducted:
Laparoscopy is a widely employed treatment for stage 2 endometriosis, a condition characterized by minimal to mild implants of endometrial tissue outside the uterus and pelvic lining. This minimally invasive surgical procedure serves a dual purpose of diagnosis and intervention.
During laparoscopy, a small incision is made near the navel, through which a thin tube with a camera (laparoscope) is inserted. The surgeon utilizes real-time visual guidance to examine the pelvic region, confirming the presence and extent of endometrial tissue growths. Upon identification, the surgeon can delicately excise or ablate these growths, removing abnormal tissue, adhesions, and cysts as needed. By addressing these tissue implants, laparoscopy aims to alleviate symptoms such as pelvic pain, painful menstruation, and discomfort during intercourse that often accompany stage 2 endometriosis. Its minimally invasive nature generally leads to quicker recovery times, reduced postoperative pain, and decreased scarring compared to traditional open surgery.
Following laparoscopy, a tailored treatment plan, potentially including pain management and hormonal therapies, may be recommended to manage symptoms and prevent recurrence, ensuring improved quality of life for individuals with stage 2 endometriosis.
According to Healthcare Bluebook, the cost of laparoscopic excision of endometriosis can vary depending on the location, healthcare provider, and type of insurance. On average, the cost of the procedure can range from $4,000 to $15,000. It’s important to note that these are estimated costs and may not reflect the actual cost you may incur.
To obtain an accurate cost estimate, it is advisable to request an appointment with NYGSE.
When addressing stage 2 endometriosis, two primary surgical options are excision and ablation, both aimed at removing or destroying endometrial tissue growths outside the uterus. Excision involves the meticulous removal of these growths, along with any associated scar tissue or adhesions. This method aims to fully eliminate the abnormal tissue, potentially providing more comprehensive relief from symptoms like pelvic pain, while also reducing the risk of recurrence. Excision is often preferred when the goal is to achieve long-term symptom management and enhance fertility, as it addresses the underlying tissue involvement.
In contrast, ablation employs techniques like heat or laser to destroy the endometrial tissue growths. While less invasive than excision, ablation may not completely eliminate all abnormal tissue, potentially leaving behind microscopic implants.
Robotic surgery is emerging as an advanced and minimally invasive option for treating stage 2 endometriosis, characterized by minimal to mild endometrial tissue growths outside the uterus and pelvic lining. This technique involves the use of robotic-assisted surgical systems, where a surgeon controls robotic arms equipped with surgical instruments to perform precise and intricate procedures. Robotic surgery offers enhanced dexterity, visualization, and maneuverability, making it well-suited for addressing endometriosis lesions with precision.
During robotic surgery for stage 2 endometriosis, small incisions are made to insert robotic arms and a high-definition camera into the abdomen. The surgeon controls the robotic arms from a console, guiding them to remove endometrial tissue growths and address any adhesions or scar tissue. This minimally invasive approach often leads to reduced postoperative pain, shorter hospital stays, and quicker recovery compared to traditional open surgery. Robotic surgery’s increased precision can aid in sparing healthy tissue and minimizing potential damage to surrounding structures, which is particularly advantageous when treating stage 2 endometriosis to alleviate symptoms like pelvic pain, painful periods, and fertility issues.
Pankaj Singhal, MD, MS, MHCM
With over 12 years of experience in both academic and private healthcare, Dr. Singhal has trained more than 45 gynecologic surgeons and fellows in minimally invasive and oncologic procedures. He has pioneered new surgical techniques for endometriosis and laparoscopic surgery, completing more than 5,700 robotic-assisted cases nationwide. Renowned for taking on the most complex cases other centers turn away, Dr. Singhal continues to advance the standard of women’s surgical care.
