Understanding the Stages 1 Endometriosis
Stage 1 endometriosis, also called minimal endometriosis, represents the earliest form of the disease. At this stage, tiny superficial implants are present on the pelvic lining or ovaries with little to no scar tissue. Although considered the least severe classification, Stage 1 can still cause symptoms, discomfort, or fertility challenges in some individuals. The following overview explains how Stage 1 endometriosis is identified, what symptoms may occur, and how it is typically diagnosed and managed.
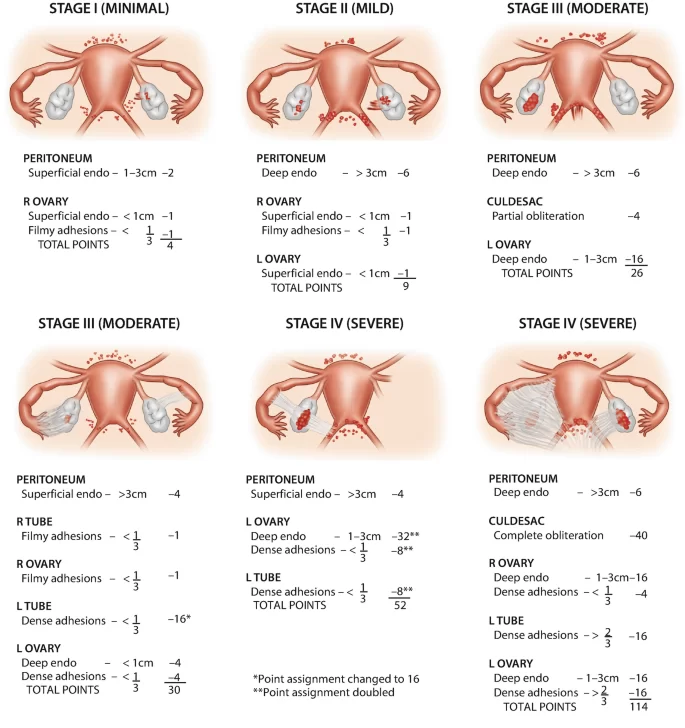
This chart illustrates how the revised American Society for Reproductive Medicine (rASRM) scoring system classifies Stage I endometriosis, also known as minimal disease.
Stage I includes a few small, superficial implants with little to no scar tissue. The scoring reflects the limited size and depth of lesions and the absence of significant adhesions or endometriomas.
While this stage indicates the least extensive disease, symptoms can still vary widely — some patients experience pain, while others have no symptoms at all.
COMMON QUESTIONS ABOUT Stage 1 Endometriosis
Stage 1 endometriosis, also known as minimal endometriosis, is the earliest and least severe form of the condition. In this stage, small patches or isolated implants of endometrial tissue are found outside the uterus, typically on the pelvic lining or ovaries. These implants are small and superficial, measuring only a few millimeters in size. At this stage, there is minimal scarring or adhesion formation.
Despite being classified as the least severe, stage 1 endometriosis can still cause symptoms and discomfort for some individuals. Common symptoms include mild pelvic pain, particularly during menstruation, and possibly pain during intercourse. However, some women with stage 1 endometriosis may have no noticeable symptoms at all.
Diagnosing stage 1 endometriosis typically involves a laparoscopy, a minimally invasive surgical procedure, during which a thin tube with a camera is inserted into the abdomen to visualize and assess the pelvic structures. If stage 1 endometriosis is detected, appropriate management options may include pain medication, hormonal therapy, or lifestyle changes. It’s crucial for individuals experiencing symptoms or fertility concerns to consult with a healthcare professional for a comprehensive evaluation and personalized treatment plan. Early detection and management can help minimize the impact of the condition on a person’s overall health and quality of life.
Stage 1 endometriosis is the mildest form of the condition, and noticeable symptoms may not always be present. However, some individuals with stage 1 endometriosis may experience the following symptoms:
- Mild Pelvic Pain: Women may experience mild, intermittent pelvic pain or discomfort, especially during menstruation (dysmenorrhea). The pain can vary from person to person and may be felt in the lower abdomen or back.
- Pain During Intercourse: Some women with stage 1 endometriosis may have pain or discomfort during or after sexual intercourse (dyspareunia).
- Mild Menstrual Irregularities: Menstrual cycles may be slightly irregular, with variations in flow or length.
- Fatigue: Fatigue or tiredness may occur during menstruation due to hormonal changes and pain.
Importantly, some individuals with stage 1 endometriosis may have no noticeable symptoms and may only discover the condition incidentally during medical evaluations for other concerns, such as infertility investigations.
It’s crucial to understand that the severity and presentation of symptoms can differ significantly among individuals.
Additionally, some women may have stage 1 endometriosis and experience severe pain, while others with more advanced stages may have milder symptoms.
If you suspect you may have endometriosis or are experiencing any symptoms of concern, it’s essential to request an appointment with New York Gynecology Endometriosis (NYGE) to seek medical advice and evaluation.
Life-threatening Complications in Stage 1 Endometriosis
In Stage 1 endometriosis, life-threatening complications are rare because the disease is in its early and least severe form. However, it’s important to note that endometriosis, regardless of its stage, can cause various health challenges and negatively impact a person’s quality of life. While life-threatening complications are not typically associated with Stage 1 endometriosis, the condition can progress over time and may lead to more severe symptoms or fertility issues if left untreated.
It’s crucial for individuals with endometriosis to seek medical attention, adhere to their healthcare provider’s recommendations, and actively manage the condition to prevent potential complications in the future. Regular follow-ups with a healthcare professional can help monitor the progression of the disease and address any emerging concerns.
The diagnosis of Stage 1 endometriosis typically involves a combination of the following steps:
- Medical History: Your healthcare provider will begin by taking a detailed medical history, including asking about your symptoms, menstrual cycle, and any previous medical conditions or surgeries.
- Physical Examination: A pelvic examination may be performed to check for any abnormalities or signs of endometriosis.
- Imaging Studies: While Stage 1 endometriosis may not always be visible on imaging, an ultrasound may be conducted to rule out other possible causes of pelvic pain and to assess the pelvic structures.
- Laparoscopy: The gold standard for diagnosing endometriosis is through a surgical procedure called laparoscopy. During laparoscopy, a thin, lighted instrument (laparoscope) is inserted through a small incision in the abdomen to visualize the pelvic organs and look for endometrial implants, lesions, or adhesions. Biopsies of suspicious areas may be taken for further confirmation.
- Histology: Biopsy samples obtained during laparoscopy are sent to a pathologist for examination under a microscope to confirm the presence of endometrial tissue outside the uterus.
Early diagnosis and intervention can lead to more effective management and improved quality of life for individuals with endometriosis.
Surgical Treatment for Stage 1 Endometriosis
Surgical treatment for Stage 1 endometriosis typically involves a minimally invasive procedure called laparoscopy. The main goals of surgical treatment are to diagnose the condition definitively and to remove or ablate (destroy) any endometrial implants or lesions found during the procedure.
Here’s how surgical treatment for Stage 1 endometriosis is usually conducted:
Laparoscopic surgery is performed under general anesthesia. A small incision is made near the navel, and a thin, lighted instrument called a laparoscope is inserted to visualize the pelvic organs and identify endometrial implants.
According to Healthcare Bluebook, the cost of laparoscopic excision of endometriosis can vary depending on the location, healthcare provider, and type of insurance. On average, the cost of the procedure can range from $4,000 to $15,000. It’s important to note that these are estimated costs and may not reflect the actual cost you may incur.
To obtain an accurate cost estimate, it is advisable to request an appointment with New York Gynecology Surgery & Endometriosis (NYGSE).
In Stage 1 endometriosis, both excision and ablation are possible surgical treatment options, depending on the specific characteristics of the endometrial lesions and the surgeon’s expertise. Here’s an explanation of each procedure:
- Excision: Excision involves surgically removing the endometrial lesions or implants. The surgeon carefully cuts away the affected tissue, ensuring that the entire lesion is removed, including any deep-seated parts. This method aims to completely eliminate the endometriotic tissue, reducing the likelihood of recurrence.
- Ablation: Ablation, also known as vaporization or coagulation, uses heat (laser or electrical energy) to destroy the endometrial lesions. The heat energy effectively destroys the tissue on the surface, but it may not penetrate deeply into the lesion. As a result, there is a higher chance of residual tissue remaining, which can potentially lead to a higher chance of recurrence compared to excision.
While both excision and ablation can be used for Stage 1 endometriosis, excision is generally considered more effective for completely removing the endometrial tissue and reducing the risk of recurrence. However, the choice of the surgical technique depends on various factors, including the size and location of the lesions, the surgeon’s expertise, and the individual patient’s preferences and needs.
Robotic surgery is an advanced and minimally invasive approach for treating Stage 1 endometriosis. During the procedure, small incisions are made in the abdomen, and a robotic surgical system is used to control precise movements of surgical instruments. The surgeon can visualize the pelvic organs in high-definition 3D, identify and remove or ablate endometrial implants, and potentially address any adhesions. Robotic surgery offers advantages such as improved precision, reduced tissue trauma, shorter hospital stays, and potentially faster recovery compared to traditional open surgery.
However, the choice of surgical approach should be discussed with a qualified healthcare professional based on individual needs and circumstances.
Pankaj Singhal, MD, MS, MHCM
With over 12 years of experience in both academic and private healthcare, Dr. Singhal has trained more than 45 gynecologic surgeons and fellows in minimally invasive and oncologic procedures. He has pioneered new surgical techniques for endometriosis and laparoscopic surgery, completing more than 5,700 robotic-assisted cases nationwide. Renowned for taking on the most complex cases other centers turn away, Dr. Singhal continues to advance the standard of women’s surgical care.
